If you’ve ever gone through the behavioral health credentialing process, you know how impactful it can be. Credentialing is your key to joining insurance networks and getting reimbursed for your services.
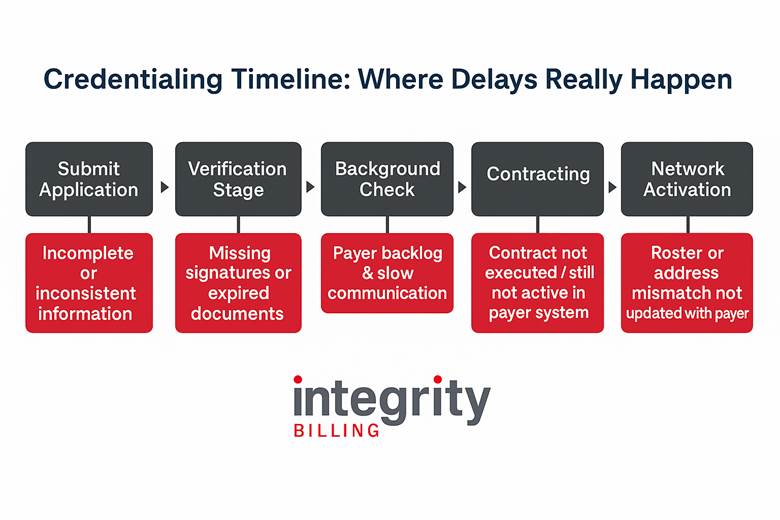
The trouble is that the credentialing process can take up to 120 days and contracts (from application to loading) up to 1 year, depending on the state. For treatment centers, that delay can mean weeks or even months without revenue. The most frustrating part? Many of the setbacks that hold up the process are avoidable.
At Integrity Billing, we’ve helped countless behavioral health organizations streamline credentialing, and we’ve seen the same hidden obstacles time and time again. Let’s break down the most common causes of delay and how to keep your applications moving forward.
Incomplete or Inconsistent Information
One of the most frequent (and easily preventable) causes of delay is missing or mismatched information. Insurance payers require exact matches across all documentation. Even a small discrepancy can trigger a system mismatch.
To avoid this setback, double check that your business name, tax ID, NPI, and address appear exactly the same on every document. Maintain a centralized credentialing folder with updated copies of all licenses, insurance certificates, and tax forms. Being organized and consistent can save weeks of back-and-forth communication.
Expired or Missing Supporting Documents
Payers require a long list of supporting materials, like malpractice insurance certificates, liability coverage, and professional licenses. If even one of these documents is expired or missing, your application can be put on hold until it’s resolved.
In behavioral health, where licenses often renew annually and insurance coverage may vary by clinician, it’s easy for something to slip through the cracks.
To keep organized, create a credentialing checklist for your organization that tracks all required documents and expiration dates. Assign one team member or credentialing partner to regularly review your records and ensure that renewals are submitted before deadlines.
At Integrity Billing, we maintain these records for our clients so payers always receive complete, up-to-date files. With us, there’s no reason to scramble to find missing paperwork!
Delayed CAQH Updates
Many behavioral health providers rely on CAQH (Council for Affordable Quality Healthcare) to store their credentialing data. While CAQH streamlines the process, it also depends on you to keep your profile accurate and current.
If your CAQH profile is missing information, expired documents, or hasn’t been re-attested within the last 90 days, payers can’t access your data, and your application will stall automatically.
We recommend setting a recurring reminder to update and re-attest your CAQH profile every 90 days. Verify that all licenses, insurance certificates, and contact information are current. If you use a credentialing service like Integrity Billing, we’ll handle these updates for you to ensure payers always have accurate data.
Payer Backlogs and Limited Communication
Even if your paperwork is flawless, credentialing can still stall due to payer backlogs. Insurance companies receive hundreds of applications every month, and their credentialing departments are often understaffed. In fact, many payers take 90 days or longer to review an application.
The best you can do here is track every application from submission to approval. Follow up with the payer every 10–14 business days, documenting each point of contact. Ask for reference numbers and the name of the representative handling your case. Without regular follow-up, it’s easy for your submission to get lost in the shuffle or sit in “pending” status indefinitely.
When Integrity Billing manages credentialing, our team tracks each submission and maintains regular communication with payers, catching delays early before they impact revenue.
Confusion Between Credentialing and Contracting
Another one of the most overlooked causes of delay is misunderstanding the difference between credentialing and contracting. Credentialing verifies your qualifications, licenses, and background. Contracting happens after credentialing, when you negotiate rates and sign an agreement to officially join the payer’s network.
Many providers assume they’re in-network as soon as credentialing is complete, but without a fully executed contract, claims will still be denied. To avoid this, confirm that your contract is signed and your information appears correctly in the payer’s system as soon as credentialing is approved. Until you’re listed as active in the network, you’re still considered out-of-network.
Staffing Changes or Missing Signatures
Behavioral health organizations often expand quickly, adding clinicians or new program types. But if staff changes aren’t communicated to payers, or if forms are missing authorized signatures, your application can hit an unexpected snag.
When adding new providers, ensure that every application includes the proper signatures and that your facility’s roster matches what’s on file with the payer. Notify insurance companies immediately of any changes to ownership, addresses, or NPIs to avoid compliance issues.
Trying to Manage Everything In-House
Perhaps the biggest cause of credentialing delays is trying to do everything yourself. Between managing staff, compliance, utilization review, billing, and patient care, keeping up with credentialing follow-ups can easily fall through the cracks. Plus, insurance companies rarely notify you if something’s missing.
Professional support can make such a difference. When you outsource credentialing to a trusted partner who understands behavioral health billing, you keep things on schedule and get reimbursed faster. Integrity Billing manages every step of the process, from organizing documentation and submitting applications to tracking progress and communicating with payers.
Faster Approvals, Fewer Surprises
Credentialing doesn’t have to be a headache. With the right systems, attention to detail, and professional support, your organization can avoid unnecessary delays and maintain steady revenue flow.
At Integrity Billing, we specialize in helping behavioral health providers streamline the credentialing and contracting process from start to finish. We know what payers look for, how to prevent bottlenecks, and how to keep your practice compliant every step of the way.
Contact Integrity Billing today at 888-368-7461 or fill out our contact form to learn how we can help you simplify credentialing for your treatment center.
